
School is back in session and the need for children/youth wearing backpacks in returning. Here are a few tips to keep their backs healthy while they carry all their books and supplies from class to class and ensure your kids don’t have any unnecessary back pain this year.
Size
- Should Not Extend Above Shoulders
- Should Rest In Contour Of Low Back (Not Sag Down Toward Buttocks)
- Should Sit Evenly In Middle Of Back
Fit
- Shoulder Straps Should Rest Comfortably On Shoulders And Underarms, With Arms Free To Move – Tighten Shoulder Straps To Achieve This Fit
- Tighten Hip And Waist Straps To Hold Pack Near Body
- Padded Straps Help Even Pressure Over The Shoulders
Weight Of Pack
- Should Never Exceed 15% Of The Child’s Weight To Avoid Excess Loads On The Spine but here are some weight recommendations
- 60 lbs child should carry max backpack weight of 5 lbs
- 60-75 lbs can carry 10 lbs
- 100 lbs can carry 15 lbs
- 125 lbs can carry 18 lbs
- 150 lbs can carry 20 lbs
- 200 lbs can carry 25 lbs
- No one should carry more thatn 25 lbs in a school backpack
Lifting Of Pack
- Proper Lifting Is Done By Bending The Knees, Squatting To Pack Level, And Keeping Pack Close To Body To Lift First To Waist Level And Then Up To Shoulders
Carrying The Pack
- Keep Both Shoulder Straps In Place And Pack Centered
- Spinal Forces Increase With Distance From The Body’s Center
Posture
- Uneven Stresses On The Spine Can Cause Muscle Imbalances. This Can Lead To Pain And Possibly Functional Scoliosis.
If your child does start to complain of constant back pain, and you have evaluated their backpack usage. Don’t hesitate to call our Pocatello clinic at (208) 233-4800.
https://ptandme.com/blog/back-pack-safety-101

Overactive bladder (OAB) is a chronic condition affecting approximately 50 million American adults, with a higher incidence in women than men. It is typically characterized by frequent and sudden urges to urinate, even if the bladder is not full. The condition can affect a patient’s sleep quality and daily functioning. OAB is NOT normal for healthy adults.
The most common symptoms of OAB are:
- Frequent urination – defined as urinating so often that it disrupts your daily life – typically 8 or more times a day
- Incontinence– partial or full loss of control of the bladder that results in leaks
- Nocturia – also known as nighttime urination, or getting up to urinate more than once per night
- Urgency – random strong desire to urinate, causing you to rush to the bathroom
How do we treat OAB?
Bladder training is a type of pelvic floor physical therapy aimed at helping a patient regain control of their bladder. It consists of retraining the patient’s bladder to hold urine for longer and longer periods of time. This allows your bladder to fill more fully and gives you more control over the urge to urinate.
How does it work?
Our physical therapists will have you keep a bladder diary to learn your bladder patterns. Keeping track of your bathroom habits may seem a little strange at first, but it is a great way for you to see trends over time and learn what types of foods and drinks trigger your incontinence, how many times you urinate, the flow of urination, was there any leakage, and did you feel an urge before voiding. Our therapists then develop a treatment plan customized to you and your symptoms that includes some of the following techniques:
- Pelvic Floor Exercises: Kegels and other pelvic exercises are designed to strengthen the muscles that control the start and stoppage of urinating. Kegels are a complex exercise that warrants training in the proper technique to improve success in delaying urination.
- Delaying urination: This is the practice of holding urine for a certain amount of time once the urge to urinate sets in. For example, a patient might start by holding it for 5 minutes, then gradually increase the time by 10 or so minutes until you can go two, three, or even four hours without urinating.
- Schedule restroom visits: This technique works by first using a bladder diary to determine how often you’re currently visiting the restroom to urinate. Start by delaying the trip by 15 or so minutes, then gradually increase the delay time in a similar fashion to the delayed urination technique.
- Diet Changes: If you’re keeping a bladder diary, you’re likely tracking what you drink or eat throughout the day to determine potential triggers for your OAB symptoms. This can help you figure out what to reduce or eliminate from your diet.
General Tips For Managing OAB Naturally
The following are general best practices for managing OAB symptoms without medication or advanced therapies:
- Always urinate right before bed and right upon waking up.
- Maintain good sleep hygiene to encourage uninterrupted sleep, regular bedtimes, and regular wake-up times.
- Avoid or quit smoking, as cigarette smoking can exacerbate OAB.
- Drink the right amount of water, a good place to start is 64 ounces – half your body weight in water.
We have pelvic floor physical therapists trained in treating OAB and are ready to help you gain control and get you feeling confident again!
https://nafc.org/bhealth-blog/how-to-manage-an-overactive-bladder/

As you start/continue your exercise program, here are a few tips to tell the difference between pain and soreness. There are many benefits to exercise. Physical activity benefits your physical, mental, and social health. Exercise improves sleep and helps you maintain strong muscles and bones. It also helps prevent or improve many chronic conditions, such as heart disease, diabetes, obesity, depression, and some cancers. When you exercise, you are putting healthy stress on your heart, lungs, muscles, and bones to gain strength or endurance. This good stress can cause normal muscle soreness and fatigue. Short-term muscle soreness is a healthy and expected result of exercise.
The good news is that normal soreness after a workout is not a cause for concern. Normal muscle soreness and fatigue peak between 24 and 72 hours after a muscle-stressing activity. It should go away on its own after a few days. But pain or discomfort that lasts may mean you have an injury.
The chart below shows the difference between muscle soreness and pain and we discuss some tips for managing both.
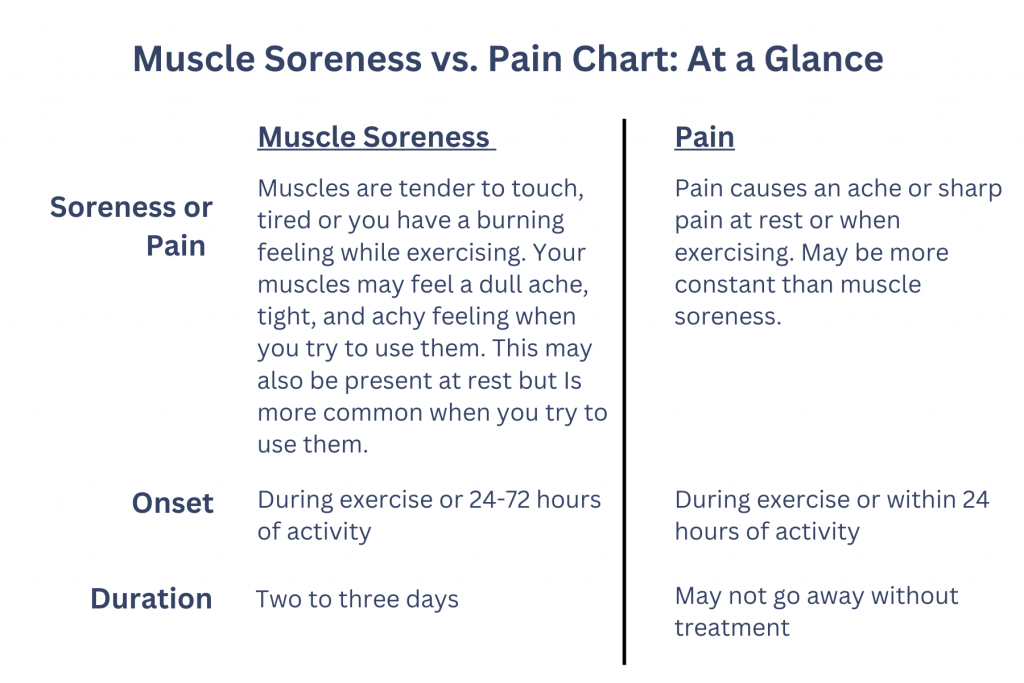
Muscle Soreness
Exercise soreness sometimes results from starting to use muscles that you have not used stressfully in a long time. This soreness is a result of small, unharmful “tearing/stress” on these unused muscle fibers. As the body repairs these small tears, muscles become stronger. Short-term muscle soreness is a healthy and expected result of exercise.
What To Do if You Have Muscle Soreness
During the recovery period, while you have soreness, it is important to:
- Give the muscles you worked time to recover. You are more likely to get injured if you continue with the same intensity and type of exercise too soon.
- Stay active and keep moving until the soreness decreases or goes away. Often improves with easy stretching and light movement. Total rest can increase soreness so while you recover, consider doing a different exercise or do your activity at a lower intensity or for less time during the first few days of soreness.
- Vary your activities. Work your legs, arms, and whole body on alternate days. This will help you keep moving and strengthen other muscles while allowing the sore ones to rest.
What To Do if You Have Pain
- Stop any painful activities and change what you do. Ice can provide short-term relief for pain caused by inflammation.
- Don’t push through the pain. Pushing through pain can cause the problem to get worse and lead to further injury.
- Seek help from a healthcare provider. If you have pain that doesn’t go away, even after 7 to 10 days, see your doctor or physical therapist for an evaluation and treatment.
How To Make Progress
Your body needs to do more than usual to make physical improvements. But you should make sure to increase your physical activity and exercise safely and slowly over time.
Each person has a different capacity to do sports and exercise. When you stay within a safe activity threshold, you should only experience normal muscle soreness. Our physical therapists can assess your strengths and weaknesses and if you have pain they can help get to the root of it. Give Meadowland Therapy a call if we can help you achieve your dreams!

Did you know physical therapy could help you poop? If you are experiencing hemorrhoids often, straining and bearing down often to have a bowel movement (BM), can’t control your urgency to have a BM, or passing gas at moments you can’t control (i.e. when walking or when moving from sitting to standing position), and/or experiencing any form of incontinence, you might be a good candidate for some pelvic floor physical therapy. Sarah Cairns, our pelvic floor physical therapist, sees both male and female patients in Pocatello with urinary and bowel incontinence. We get questions from patients about having healthy, regular bowels so we wanted to share some practical tips.
The ideal frequency is up for debate. Our frequency goal for patients is a consistent schedule with ease and no straining. Bowel movements should be soft and easy to pass, with no pain, straining, or stool leakage. Establish a healthy bowel routine by checking in with yourself to see if you are doing some of these tips. If not, can you improve a few of the following?
Tips for good bowel health
- Go when your bowel is most active (first thing in the morning and after meals) and when you feel the urge.
- Eat a healthy diet including foods high in fiber such as whole grains, fruits, and vegetables.
- Cut out irritating foods such as caffeine, dairy, processed meats, sugar, carbonated beverages, and artificial sweeteners.
- Drink 8 glasses of water daily.
- Eat regularly and don’t skip meals. The bowel functions best when it is introduced food at the same regular intervals.
- Get active to help move food through the digestive tract.
- Allow enough time on the toilet so you don’t need to rush or strain.
- Use the best position for emptying your bowels: lean forward, with a straight back, forearms on your thighs, and feet slightly raised if possible (you may find a footstool helpful).
- Do not hold your breath while trying.
- Be aware of your bowel habits so you notice when something changes.
- Maintain a healthy weight and don’t smoke because obesity and smoking are associated with an increase in the risk of bowel cancer.
If you are experiencing any pain, consistency changes, and/or are infrequent or difficult to pass, give our clinic a call! We can help teach you techniques to improve your overall bowel health, which improves your quality of life!

Do you or someone you know experience kneecap pain with the following activities?
- Squatting (with or without weight).
- Climbing or going down the stairs.
- Sitting for a long time.
- Running, especially downhill.
- Jumping.
About 25% of Americans will feel this type of kneecap pain, known as patellofemoral pain. More women than men will have it, and it affects people of all ages, heights, and weights.
Kneecap pain can be hard to prevent and is a result of one or more of the following:
- Increasing the load and/or frequency of knee loading faster than your knee can adapt.
- Lack of strength in the muscles on the front of your thigh.
- Specializing in a single sport.
- Certain hip and knee movement patterns.
There are no quick fixes for kneecap pain, but there is hope. Exercise, along with other treatments by a physical therapist when appropriate, has been proven to reduce or eliminate kneecap pain.
Our physical therapists will perform an initial exam and develop a treatment plan specific to your body and its needs. This treatment plan will use exercises that target the hip and knee muscles to help you recover from kneecap pain. Most importantly, our physical therapists want to get you back out doing what you love, pain-free.
Here are five tips to help prevent or reduce kneecap pain.
1. Address Hip Strength.
Do hip strengthening exercises, such as squats, lunges, leg presses, and step-ups, slowly adding the amount of weight support and knee motion during the exercises over time. If this causes pain, call a health care professional.
2. Strengthen Quads.
Include non-weight-bearing knee extension exercises to strengthen the muscles on the front of your thigh, along with hip exercises, to boost strength in the muscles that support your knee.
3. Use arch Supports.
Try low-cost shoe inserts for arch support combined with exercise, but only for the first few weeks (up to six) until your muscles are stronger. Shoe inserts are available from pharmacies or athletic shoe stores. Custom-made shoe inserts are no more effective than shoe inserts available over the counter.
4. Add Variety to Your Activities.
Vary the types of activities you do (walk, swim, bike, run) so that you don’t overuse certain muscle groups. Young athletes who specialize in a single sport have a higher risk of kneecap pain.
5. Avoid Braces and Knee Straps.
Although they may temporarily reduce your pain, over-the-counter knee braces, sleeves, or straps do not address the causes of kneecap pain. A physical therapist can work with you to address any muscle imbalances or movement problems that may contribute to your knee pain.
Getting help early is key. If you still feel pain after a couple of weeks then call a physical therapist or doctor for help. Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. Give us a call at Meadowland Therapy (208) 233-4800 in Pocatello for help!
https://www.choosept.com/health-tips/kneecap-pain-5-research-backed-tips-get-better

Many men go into surgery thinking that once the prostate is removed their problems will be solved. Sometimes this is true and sometimes it is not. We want you to know what you should know so you can be prepared.
Here is an example:
Alan was 68 years old when he had a prostatectomy. “My doctor thought it was the best way to treat my prostate cancer and I agreed”, he said. “We talked about the risks involved, how to prepare for the surgery, and what would happen during the surgery, but it was what happened after prostate surgery that I didn’t expect. He never told me about the potential for bladder leaks.”
“I thought it was probably normal to have some incontinence after prostate surgery, but 6 weeks after I had the catheter removed, I was still unable to stand up without leaking urine. I’ll never forget the day I had my catheter taken out. I came home, had a beer to celebrate, and immediately it all just rushed out of me when I stood up a half-hour later. I just didn’t expect this to happen and was really worried that it was going to become a permanent part of my life.”
“I went in for a checkup, and that’s when my doctor told me that this is a common side effect for some men. He told me that the leaks would likely recover with time, and he went through my options and discussed what I could do to help speed up the recovery process, which was helpful. I just wish he would have told me all this sooner, before the surgery. At least then, I could have known what to expect.”*
Alan is not alone in this. It is common to experience incontinence after prostate surgery but it is NOT normal for it to linger long.
WHAT CAUSES INCONTINENCE AFTER PROSTATE SURGERY?
Urinary incontinence is a possible side effect of prostate removal surgery. The prostate is located just below the bladder and surrounds the urethra. Removing it, or using radiation to treat it, can sometimes cause damage to the nerves and muscles of the bladder, urethra, and or sphincter, which controls the passage of urine from the bladder. This can result in urinary incontinence. Most times this type of incontinence is stress incontinence, which occurs when pressure is placed on the bladder. Activities like sneezing, coughing, working out, lifting, jumping, and even standing up can cause you to leak urine.
IS INCONTINENCE NORMAL AFTER PROSTATE SURGERY?
Bladder leakage after prostate removal is not all that uncommon and typically will go away after your body begins to heal and your muscles regain strength. Approximately 6-8 percent of men who have had surgery to remove their prostate will develop urinary incontinence. (Cleveland Clinic) The good news is that most men will eventually regain bladder control with time.
HOW BAD IS INCONTINENCE AFTER PROSTATE SURGERY?
It depends! It can be anywhere from full-on incontinence, to light dribbles. Some men may only experience this with certain activities, like working out, whereas some may experience leaks when going from sitting to standing.
HOW LONG WILL I HAVE INCONTINENCE AFTER PROSTATE SURGERY?
Men will typically have a urinary catheter (a tube) inserted which will help drain the urine from the bladder after the surgery. The catheter is needed until the urethra heals, which typically takes anywhere from 1-3 weeks. After the catheter is removed, it can take several weeks or more to completely stop leaking. Most men who experience a loss of bladder control have symptoms for 6 months to 1-year post prostate surgery. However, a small percentage of men may continue to experience problems past the one-year mark.
DOES INCONTINENCE GO AWAY ON ITS OWN AFTER PROSTATE SURGERY?
For most men, urinary incontinence will go away within about 1 year but can vary depending on the severity of your incontinence, and how/what you are doing to manage it. Some men may recover from leaks within weeks, whereas others will take months for the bladder leaks to subside. Performing pelvic floor exercises, such as Kegels, or attending pelvic floor physical therapy can help strengthen the muscles to help speed the recovery process along.
We have therapists who specialize in pelvic floor physical therapy and want to get you confident and doing what you love with no worries that leakage would interfere. Give us a call (208)233-4800 if we want help!
*https://www.nafc.org/bhealth-blog/urinary-incontinence-after-prostate-surgery-everything-you-need-to-know


